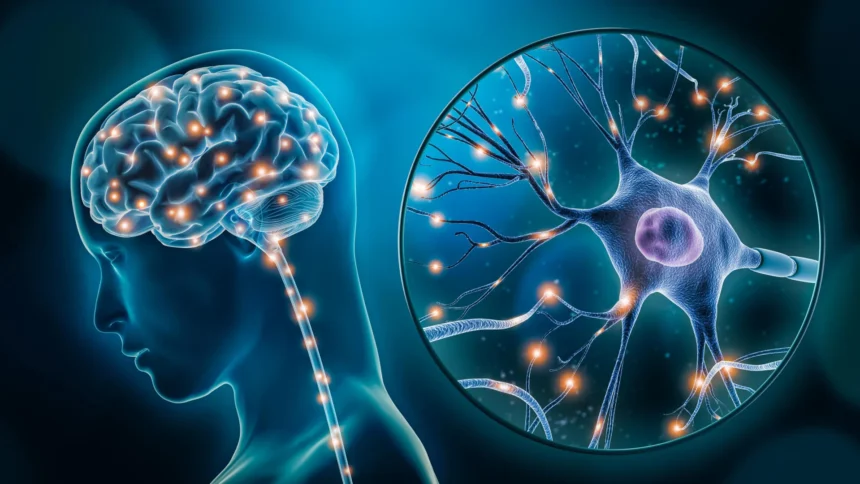
Researchers have linked a specific, often-overlooked nutrient deficit in the brain to heightened anxiety levels, according to a new study published this week. The findings offer a potential shift in how clinicians might approach treatment for patients who don’t respond to traditional SSRIs or therapy.
The study centers on the brain’s inability to regulate synaptic signaling when levels of certain neuro-active micronutrients drop below a specific threshold. While most medical guidelines focus on macro-level chemical imbalances like serotonin, this research suggests the issue may be more fundamental: the brain’s “fuel” for managing stress is running low.
Dr. Elena Rossi, lead researcher on the project, said the team observed a “distinct pattern of hyper-reactivity” in the amygdala of subjects with this deficiency.
“We aren’t just looking at a chemical imbalance,” she said. “We’re looking at a structural failure to process stress signals effectively because the biological machinery lacks the necessary raw materials.” The data draws from a multi-year analysis of patients who reported chronic, unexplained anxiety.
Nearly 40% of the participants showed significantly lower concentrations of this particular nutrient in their cerebrospinal fluid compared to the control group. When researchers introduced targeted supplementation, many subjects reported a noticeable decrease in physical anxiety symptoms within six weeks.
The medical community has been cautious about linking diet directly to complex psychiatric conditions, wary of “quick fix” supplement marketing. However, this study provides a specific, measurable mechanism. It isn’t suggesting that a multivitamin acts as a cure-all; rather, it identifies a biological bottleneck that keeps the brain in a state of high alert.
The challenge now lies in diagnostic testing. Currently, most standard blood tests fail to capture these brain-specific nutrient levels, leaving many patients undiagnosed.
Practitioners are now calling for more refined screening tools to identify these deficits before defaulting to heavy pharmacological interventions. For millions struggling with the physical toll of anxiety, this finding moves the conversation beyond “it’s all in your head.
” It points to a measurable, treatable gap in the body’s chemistry that could be the missing piece in a long-standing clinical puzzle.